There was a time when the sharp buzz of a pager and a short code like “Code Blue” was one of the most reliable ways to reach a medical team inside a hospital. Everyone knew the sound. Everyone knew what it meant. Pagers became a symbol of clinical readiness – simple, immediate, universally understood.
The limitations of that simplicity, however, have become impossible to ignore.
A pager delivers almost no context. A short code and a phone number. Nothing more. Even when clinicians know every possible code by memory, the message itself rarely explains what is actually happening. Is this an emergency or a routine update? A clinical issue or an administrative request? A critical situation or a non-urgent follow-up? Each unanswered question costs time – and in healthcare, time directly affects outcomes.
Worse, multiple alerts arrive simultaneously. Over time, alert fatigue sets in, and clinicians begin to delay responses or tune out signals altogether. What starts as a usability problem quietly becomes a patient safety risk. And beyond fatigue, traditional paging systems offer little protection against interception or unauthorized access – a growing concern in an era of tightening compliance requirements.
Many healthcare organizations are aware of these gaps and still haven’t closed them. The reason is rarely a lack of commitment or expertise from care teams. It is the tools they are forced to use. Research from CRICO Strategies, analyzing 23,000 malpractice lawsuits, found that over 7,000 cases were linked to communication failures – contributing to nearly 2,000 preventable deaths and $1.7 billion in malpractice costs.
Modern healthcare organizations are responding by rethinking how their teams communicate at every level: not just at the point of care, but across departments, between shifts, and among roles that rarely share the same physical space. The infrastructure supporting that coordination matters as much as the clinical systems themselves.
This article explores what that shift looks like in practice – what clinical communication software is, who relies on it, what genuine HIPAA compliance requires, and how organizations are evaluating their options. We will also look at where dedicated team coordination tools fit alongside clinical systems, and why that distinction is becoming more important as care delivery grows more complex.
Let’s start with the core question. Why does clinical communication matter more today than ever before?.
Part 1: Understanding clinical communication
What is clinical communication?
Clinical communication is the structured exchange of information that enables safe, effective, and coordinated patient care. It ensures that patients, carers, and healthcare professionals share the right information at the right time, with accuracy, clarity, and respect.
Every minute, clinical communication is happening in practice. A surgeon cannot start an operation without coordination with the anesthesiologist. After every shift change, a nurse must collect and hand off critical details. The same applies to pharmacists, who need to confirm dosages with doctors to prevent adverse reactions. These interprofessional interactions connect individual actions into a single treatment plan and directly influence patient outcomes.
Unlike casual workplace communication, clinical communication carries high stakes. There is no room for delays or uncertainty between departments, as even small gaps can affect care decisions. Precision and timing are essential to patient safety.
Clinical communication is not a soft skill. It is a professional competency shaped by strict privacy regulations such as HIPAA, complex medical terminology, and constant time pressure. It also extends beyond clinical teams to doctor-patient conversations, where clarity and empathy support informed consent, trust, and better health outcomes.
When clinical communication breaks down, patients are put at risk. This is why healthcare organizations are increasingly investing in platforms designed to support secure, real-time collaboration — tools that protect sensitive data, reduce the risk of errors, and give care teams the clarity they need to act confidently. What those tools look like varies widely depending on the environment, the team size, and the specific problems being solved.
5 Key principles of clinical communication
The pace of healthcare is relentless. In the rush of handovers, consultations, and cross-department updates, clinical communication must function as an integral part of daily operations.
To be effective, it must be guided by a few core principles:
- Clarity – Every message should be sharp, direct, and actionable. Misunderstandings can lead to errors; clarity prevents them.
- Speed with precision – Information must flow in real time but never at the cost of accuracy. The right person needs the right message at the right moment.
- Contextual relevance – Communication must be tailored to its audience. A nurse’s needs differ from those of a surgeon or pharmacist. Messages should be aligned with task, role, and urgency.
- Security – Patient data must be protected at all times. HIPAA compliance is not a box to tick – it’s a foundation of trust.
- Empathy and professionalism – Even under pressure, communication must remain professional and compassionate. Precision matters, but so does tone.
Specialized clinical communication software helps teams follow these principles by providing secure, reliable alternatives to standard messaging or phone calls.
What clinical communication requires from providers and patients – and the role of HIPAA
Knowing what makes clinical comms effective is only part of the story. The deeper question is: What does it ask of the people involved?
For healthcare professionals, it’s not enough to be fast and clear. Every interaction also requires presence – balancing urgency with empathy, and precision with emotional awareness. Good clinical communication means listening actively, explaining treatments in plain language, clarifying consequences of medical decisions, and checking the patient’s perspective. Non-verbal cues matter too: posture, eye contact, or a simple nod can make a difference. Building trust, exchanging information mutually, supporting shared decision-making, and navigating uncertainty are all part of the daily routine .
Patients, too, play an active role. They bring fear, confusion, questions – and a fundamental right to understand what’s happening. Clinical communication should serve as a bridge, connecting patients to their care teams with transparency, inclusion, and dignity.
Holding it all together is HIPAA – the invisible framework that ensures communication stays ethical, legal, and secure. More than paperwork, it defines how information is shared, stored, and protected. For providers, that means every message, system, and tool must follow strict data privacy rules. And in today’s digital world, it’s no longer just about compliance – it’s about fostering a culture where privacy, safety, and clarity coexist in every interaction. Choosing platforms with strong clinical communication features ensures that these standards are met consistently, from secure messaging to audit trails and controlled access.
Part 2: Clinical communication software and collaboration platforms
So far, we’ve explored the critical nature of clinical communication, its complexity, and how deeply it is woven into everyday healthcare. What’s clear is that this is no longer a function that can be left to chance or managed by outdated solutions, even if some still carry a sense of nostalgia.
For a long time, healthcare teams relied on phone calls, handwritten notes, and pagers to get through the day. To be fair, those tools did their job. In certain situations, such as power outages or network failures, they can still act as a basic safety net. Pagers have even evolved and remain surprisingly reliable in environments with limited connectivity.
But these tools were never meant for the constant, high-stakes collaboration modern healthcare demands. Their use left medical staff guessing:
- Did the pager alert reach the right person?
- Did the paper get lost between departments?
- Is someone acting on it right now?
- Where did the patient’s data end up?
- Could the clinic face litigation for exposing PHI?
That uncertainty doesn’t end when a shift does – it follows clinicians home, keeps them mentally on call, and makes it hard to truly rest.
Clinical communication software exists to remove that uncertainty.
It is a digital system designed to support secure, efficient, and contextual information exchange among healthcare professionals. These platforms act as centralized hubs, allowing teams to share messages, alerts, updates, and patient-related information in real time within a single environment.
Unlike traditional tools, clinical communication software is built for safety and accountability. These platforms are designed to make every step of communication traceable, secure, and efficient, so teams can act confidently and quickly.
- Message history is traceable – you can always double-check a treatment plan, follow up on previous instructions, and see the full conversation trail, which reduces mistakes and ensures accountability.
- Confirmed status – the “read by” confirmation takes the guesswork out of messaging, so you can stop pulling your hair out wondering if a critical alert reached the right person.
- Notifications can be tuned – only essential alerts come through, helping you prioritize urgent tasks and avoid the mental drain of alert fatigue.
- Sensitive information is protected – patient data and lab results remain visible only to authorized staff, letting clinicians rest easy knowing compliance standards like HIPAA are respected.
- Collaboration across departments – clinicians can share context, attach files, and coordinate complex workflows seamlessly, ensuring that every team member stays on the same page even in high-pressure situations.
These tools are fully integrated collaboration systems that support real clinical workflows – not just message delivery. Clinicians can share context, attach files, coordinate across departments, and trust that communication is secure, compliant, and complete.
That said, not all clinical communication platforms are built for the same problems. Some are designed deep inside clinical workflows – tightly integrated with EHR systems, built for acute care environments, and focused on point-of-care communication between physicians and nursing staff. Others are built for the coordination layer that surrounds those systems: the shift handoffs, cross-department task management, scheduling conversations, team announcements, and interprofessional communication that clinical systems were never designed to handle.
Both categories are legitimate. Both solve real problems. But confusing them leads organizations to evaluate the wrong tools against the wrong criteria. The comparison below covers both, and we’ve noted which category each platform primarily serves.
The best clinical communication software
The platforms below fall into two broad categories. Clinical integration platforms are built around EHR connectivity and acute care workflows – they’re designed to live inside the clinical system ecosystem. Team coordination platforms focus on the interprofessional and operational layer: how care teams communicate, coordinate tasks, share documents, and stay aligned across departments and shifts without necessarily touching patient records directly. Most organizations benefit from understanding both, since they solve different problems and often complement each other.
| Feature | Chanty | TigerConnect | symplr (Halo Health) | Connecteam | OnPage | Buzz Messenger | Microsoft Dragon Copilot |
|---|---|---|---|---|---|---|---|
| HIPAA & GDPR Compliance | Full compliance | Full compliance | Full compliance | Full compliance | Full compliance | Full compliance | Full compliance |
| Secure Messaging & Encryption | End-to-end encryption | Secure messaging | Secure messaging | Secure messaging | Secure messaging | Secure messaging | Secure messaging |
| Real-Time Instant Messaging | Fast and intuitive chat | Robust messaging | Messaging + alerts | Mobile messaging | Critical alerting | Messaging | Messaging + AI features |
| Task & Workflow Management | Built-in Kanban-style boards | Task management | Task and scheduling features | Task checklists | ❌ | Basic task features | Task & documentation |
| Mobile & Desktop Apps | Fully optimized and mobile-friendly | Fully optimized | Fully optimized | Mobile-focused | Mobile & desktop | Mobile-friendly | Desktop & mobile |
| Ease of Use & Onboarding | Intuitive, minimal training | Medium complexity | Medium to high complexity | Medium complexity | Medium complexity | Easy to use | Medium complexity |
| Integration with EHR Systems | Custom integration via API possible | Native EHR integration | Native EHR integration | Limited | Limited | Limited | Native EHR integration |
| Advanced Security Features | IP Allowlist, 2FA, DLP | Basic to advanced features | Advanced compliance features | Basic compliance | Escalation & confirmations | Basic compliance | Advanced AI security features |
| Collaboration Features | Chat, video calls, polls, announcements | Messaging + alerts | Messaging + scheduling | Messaging + checklists | Critical alerting | Messaging + voice/video | Messaging + AI documentation |
| Focus / Best Fit | Interdisciplinary teams needing secure, simple communication | Large hospitals with enterprise needs | Acute care hospitals with complex workflows | Mobile frontline workers | Rapid incident response teams | Small to mid-sized clinics | Providers needing AI-powered documentation |
Connecteam
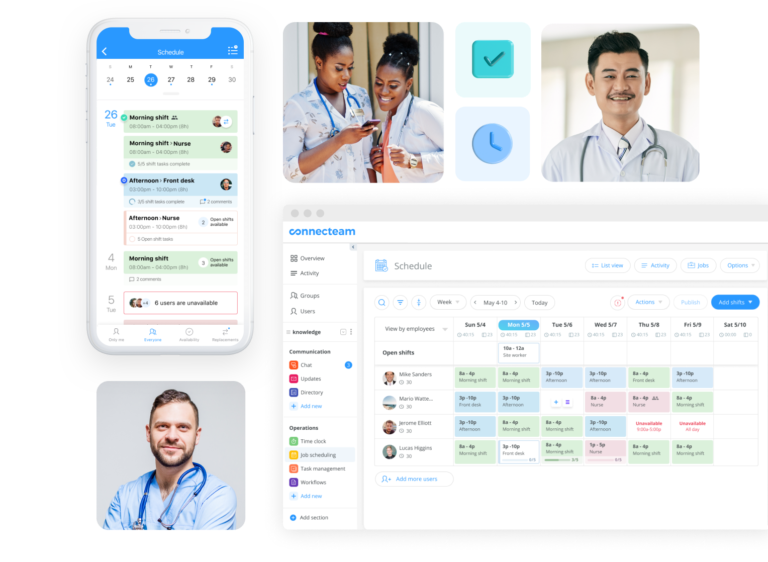
Ideal for: Nurses, home health aides, and multi-site support teams.
Connecteam is designed with frontline healthcare workers in mind. It centralizes essential communication with HIPAA-compliant chat, customizable forms, and digital checklists – perfect for mobile staff who need instant updates on the go. Supervisors can assign and track tasks, ensuring accountability without chasing paperwork. It’s especially useful in settings like long-term care facilities, home health services, or large clinics where not everyone is desk-based.
- Why it fits: Empowers mobile teams to stay connected, organized, and compliant – even when they’re on different floors, shifts, or sites.
TigerConnect
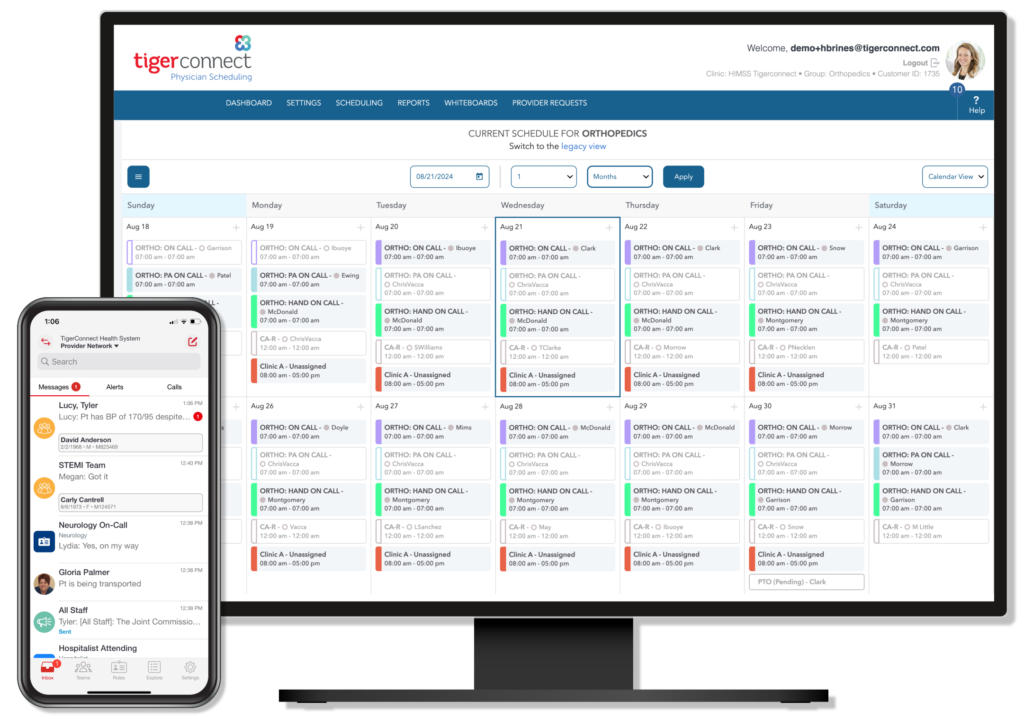
Ideal for: Physicians, hospitalists, specialists, and care coordination teams.
TigerConnect enables seamless communication across departments and roles. Its integration with EHR systems allows clinicians to send patient updates or lab results in real time. Nurses can alert physicians without relying on pagers, while administrators benefit from advanced analytics on communication flow.
- Why it fits: Reduces communication lag in hospitals and emergency settings, improving care transitions and response time – a must-have for large institutions or those managing critical care.
symplr

Ideal for: Charge nurses, care coordinators, and on-call scheduling teams.
Built specifically for acute care environments, symplr handles the intricate coordination required in hospitals. It simplifies complex on-call scheduling, letting teams know who’s available instantly – no need to flip through paper charts or chase down colleagues. Its secure chat and alert features also help reduce care fragmentation.
- Why it fits: Streamlines care team communication and shift coordination, helping ensure no patient or task falls through the cracks in high-pressure settings.
OnPage

Ideal for: Rapid response teams, IT incident managers, and clinical leadership.
OnPage is more than just secure messaging – it’s built for critical communications. With built-in escalation rules and delivery confirmations, it ensures alerts are never missed. For example, a nurse can trigger an urgent cardiac alert that will escalate to the next available provider if there’s no response.
- Why it fits: Perfect for high-risk workflows, like critical care or behavioral health, where timing is everything and accountability needs to be traceable.
Buzz Medical Messenger by Skyscape
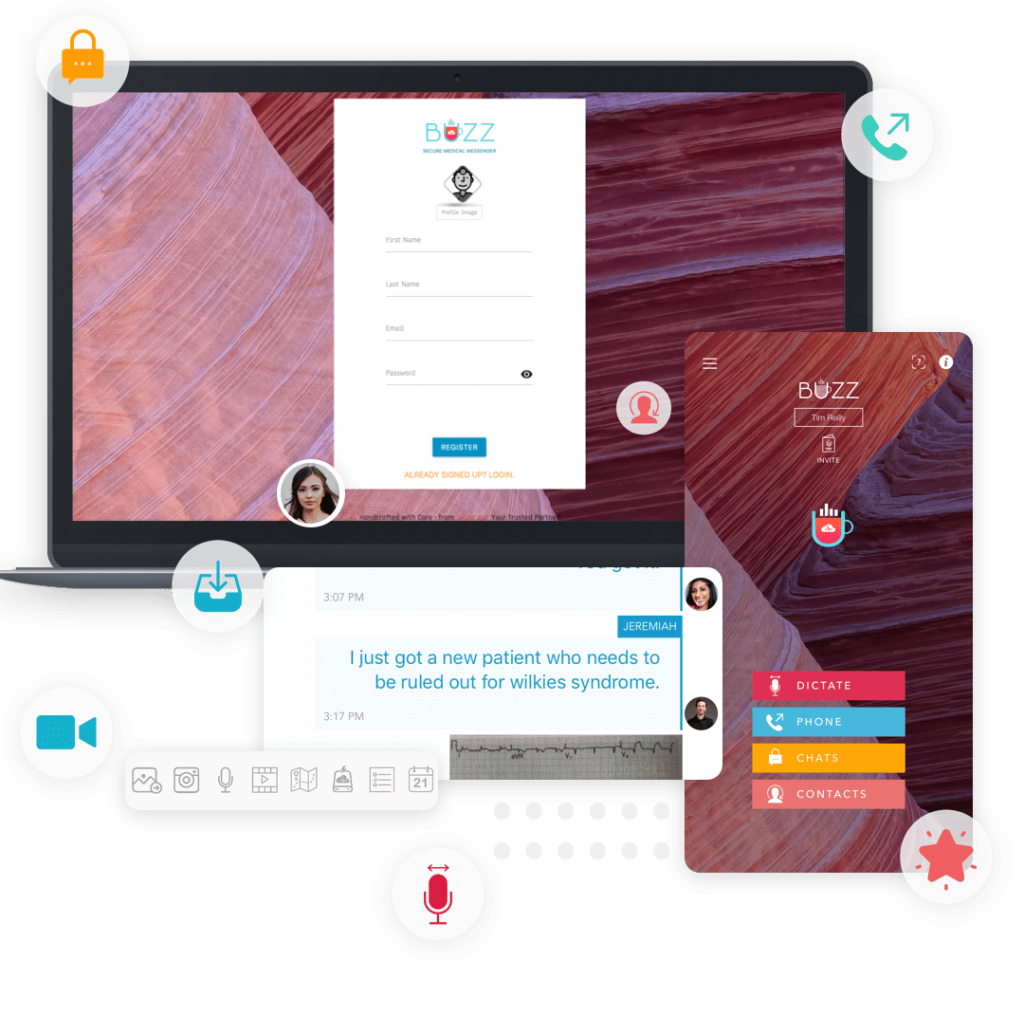
Ideal for: Private practices, outpatient teams, and telehealth providers.
Buzz is lightweight, intuitive, and easy to deploy. It combines HIPAA-compliant texting, group messaging, and even voice and video options. Small clinics or specialty providers can use it to stay in sync without overwhelming staff with overly complex systems.
Microsoft Dragon Copilot
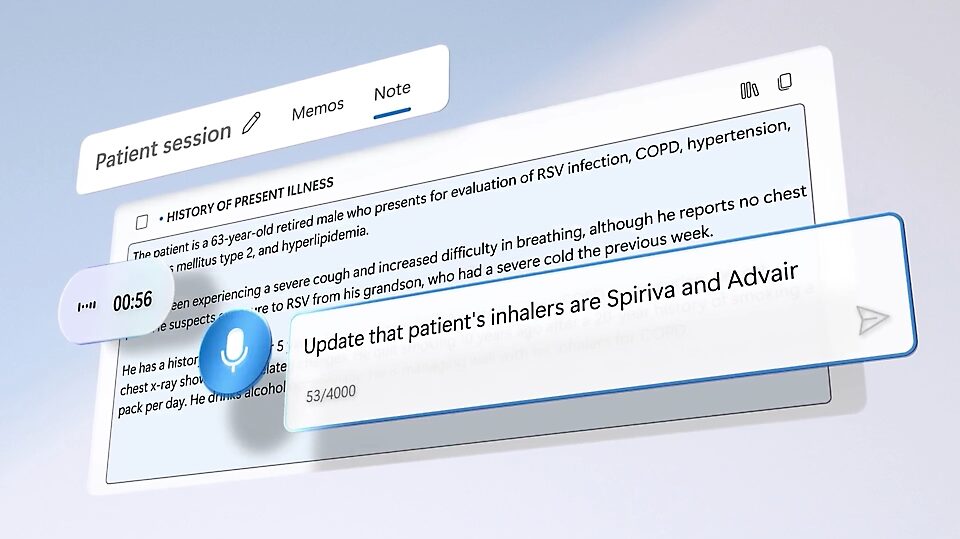
Ideal for: Physicians, nurse practitioners, and administrative staff.
Dragon Copilot brings AI into the daily routine of clinical documentation. With voice recognition and ambient listening, it captures conversations and auto-generates progress notes, freeing clinicians from typing or dictating notes later. It integrates with EHRs, helping reduce burnout while maintaining compliance.
- Why it fits: Transforms how providers interact with records and documentation – saving time, reducing errors, and allowing more focus on patients.
Why Chanty could be the perfect option for clinical teams
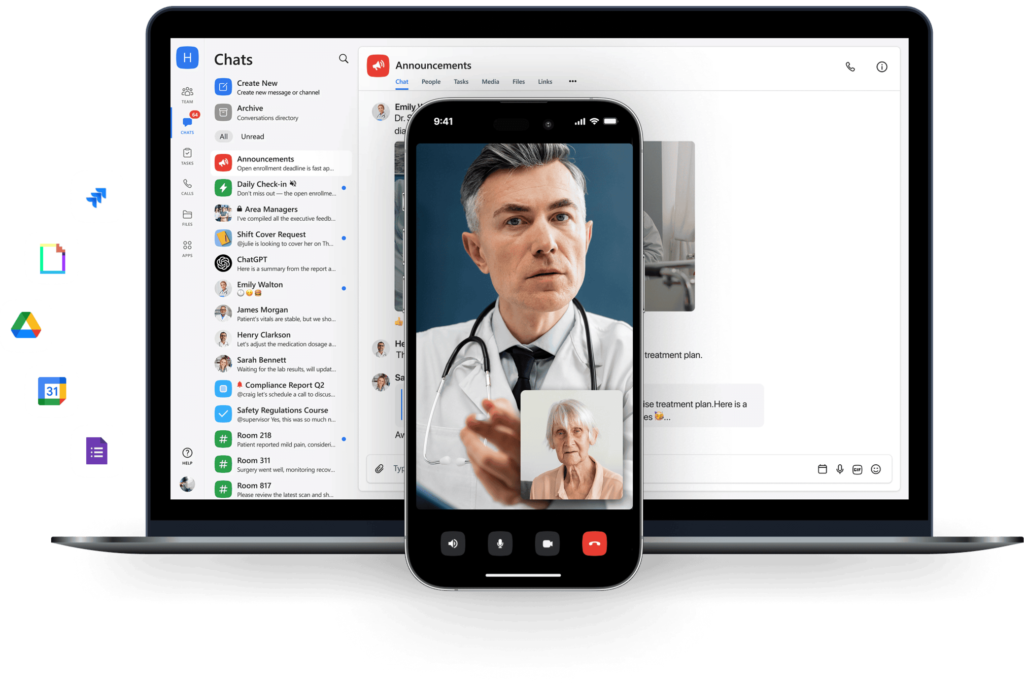
Chanty isn’t a clinical records system and doesn’t try to be. What it does is handle everything that happens between those systems – the scheduling conversations, the cross-department task handoffs, the shift announcements, the quick video calls, and document shares that hold a care team together across a twelve-hour day.
We deeply understand the challenges medical professionals face: managing complex workflows, safeguarding sensitive patient data, coordinating across multiple departments and locations, and juggling clinical responsibilities alongside administrative tasks. Chanty helps reduce these burdens by delivering real-time communication that keeps your entire care team aligned and focused on what matters most – the patients.
What HIPAA compliance looks like in practice
Chanty is fully HIPAA compliant and provides a Business Associate Agreement to every healthcare customer – not as an add-on, but as a standard part of onboarding. On the security side, that means end-to-end encryption on all messages, an IP Allowlist that restricts workspace access to authorized networks only, two-factor authentication, and data loss prevention controls. One-to-one messages are strictly private. Every conversation is logged and traceable, which matters both for compliance audits and for the simple operational need of knowing what was said, when, and by whom
What a typical day looks like
A morning shift coordinator opens Chanty and posts the day’s staffing update to the relevant department channel – visible to the right people, not the whole organization. A charge nurse assigns three follow-up tasks from the overnight notes directly in the same thread, with owners and due times attached. A pharmacist sends a quick message to confirm a dosage change with the attending physician, who responds from their phone between rounds. None of this touches the EHR. All of it is encrypted, logged, and HIPAA compliant.
That’s the coordination layer – the part of the day that clinical systems don’t cover and personal messaging apps shouldn’t.
Who it fits best
Chanty works well for outpatient clinics, home health agencies, rehabilitation centers, specialty practices, and any care environment where the primary communication challenge is team coordination rather than EHR-integrated clinical alerting. It’s also a practical fit for the administrative and operational staff within larger hospital systems who need a secure, simple tool that doesn’t require IT-level onboarding.
If you’re running a large acute care hospital and need deep EHR integration and clinical escalation protocols, the platforms listed above, TigerConnect, symplr, OnPage, are built specifically for that environment. Chanty is the right conversation if your team is currently coordinating on tools that aren’t compliant, or if you need a secure, affordable platform that people will actually use without a training program.
Pricing starts at $3 per user per month. A Business Associate Agreement is included. If you want to see what it looks like for your team’s specific setup, we’re happy to walk through it.
Book a no-pressure demo today – let’s explore how Chanty can simplify communication and help your clinical staff focus on what really matters.
Wrapping up
In the ever-evolving world of healthcare and life sciences, clinical communication is no longer just a support system – it’s a living, breathing part of patient care. From understanding what clinical comms truly is, to navigating the principles it stands on, and finally choosing the right tools to sustain it, we’ve traveled through the very heart of how modern care teams stay connected.
What becomes clear is this: technology may carry the message, but it’s the people who shape the meaning. Clinical communication software and collaboration platforms are here to serve, not complicate, the essential work being done every hour of every day. But using them responsibly is not optional. With the sensitivity of patient data and the high stakes of clinical decisions, the tools we choose must be paired with a deep understanding of how to use them safely.
So, a few ground rules worth keeping close:
- Only use HIPAA-compliant platforms when handling patient information. This is your legal and ethical shield.
- Be cautious with permissions. Not everyone needs to see everything. Tailored visibility keeps information precise and secure.
- Avoid personal devices or unsecured apps for professional communication, unless you’re sure they meet the standards.
- Educate your team – clinical communication is only as strong as its weakest link.
- Regular audits and reminders help keep good habits fresh and reduce risk over time.
When communication technology is used thoughtfully, it becomes a trusted partner – helping your team respond faster, coordinate better, and ultimately deliver safer, higher-quality care.
The tools your team uses to coordinate – not just to document – shape the quality and safety of care in ways that are easy to overlook until something goes wrong. Choosing them thoughtfully, with an honest understanding of what each tool is actually designed to do, is part of running a responsible clinical environment.
If your team’s day-to-day coordination is still happening on personal phones or unencrypted group chats, Chanty is worth a look. It’s a straightforward platform – secure, HIPAA compliant, and built for the kind of interprofessional communication that keeps a care team functioning between the clinical moments. If it sounds like a fit, book a demo, and we’ll walk you through how it works for your team.